An ultrasound examination (photo: Jan Chlebik/the ICR)
Puzzling over bats flying at night, Lazzaro Spallanzani — an Italian biologist and physiologist — was one of the first to investigate how ultrasound worked back in the 1790s.
Blindfolding the bats did not stop them navigating through the night, but when their ears were plugged they started bumping into obstacles. Spallanzani concluded that their primary mode of navigation was mediated through waves that echoed off of objects and helped to determine their distance.
Fast-forward around 200 years and we are now using ultrasound in an array of cutting-edge medical applications, including finding, diagnosing and treating cancer.
New ultrasonic imaging techniques
Here at The Institute of Cancer Research, London, Dr Emma Harris and the Imaging for Radiotherapy Adaptation Team are developing various novel ultrasonic imaging techniques to help plan and guide the delivery of radiotherapy and to predict and monitor treatment response.
One of Dr Harris’ projects is using ultrasound to assess changes in breast tissue linked to radiotherapy. Because more women are now surviving breast cancer due to improvements in treatments, late side-effects from radiotherapy are becoming more apparent.
Around 20% of women who receive breast radiotherapy will experience breast hardening or shrinkage. Researchers think that the likelihood of developing these reactions is down to the individual genetic make-up of patients.

But in order to identify these genetic differences, we need to quantify accurately the severity of these side-effects.
Dr Harris says: “So far, clinicians have judged the severity of the symptoms through touch and visual appearance. But these clinical methods are subjective and can vary greatly. For example, clinical assessment often fails to distinguish between swelling — an early transient effect — and hardness, which develops later and is usually permanent.
“Because of this, we have difficulty in pooling data from different studies, which is an essential approach for investigating genetic susceptibility.”
Ultrasound techniques, however, may be able to help quantify and characterise radiotherapy-associated changes to a higher specificity in breast tissue, allowing researchers to link these with genetic abnormalities.
Pilot studies
Collaborating with Dr Jeff Bamber at the ICR, Dr Anna Kirby’s team at The Royal Marsden NHS Foundation Trust, and clinicians in Addenbrookes Hospital in Cambridge, Dr Harris is conducting the QuaRTUS trial — a pilot study that’s investigating whether an ultrasound-based imaging technique can measure tissue stiffness accurately.
Researchers are using two approaches: ultrasound backscatter spectroscopy and shear-wave elastography.
Ultrasound backscatter spectroscopy uses the frequencies of ultrasound reflected by tissues to characterise tissue structure, and has already been tested in a breast tissue. Although the technique was able to detect some damage, measurements were difficult to obtain because of variation in ultrasound signal due to differences in breast tissues.
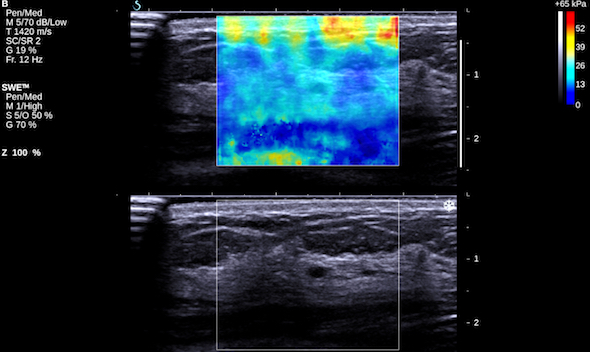
Breast ultrasound image from a healthy volunteer with elastography information overlaid in colour acquired using Aixplorer – a system that incorporates shear wave sound speed to measure stiffness in breasts. Stiffness is represented by the colour spectrum ranging from dark red (very stiff) through to blue (very soft), and shows higher stiffness in the skin region and lower stiffness in subcutaneous fat. Grey scale image shows a mixed echo texture due to varying tissue architecture in the breast (image: Dr Emma Harris).
Using ultrasound shear-wave elastography, which measures tissue stiffness and stretchiness, does not suffer these problems and may be a preferable alternative.
Dr Harris explains: “Patients who have swelling or hardening of breast tissue after radiotherapy will be tested using the two techniques. We believe that the ultrasound shear-wave elastography will be able to distinguish between swelling and hardness, and will help us determine side-effects from radiotherapy more accurately than ultrasound backscatter spectroscopy. We are eagerly looking forward to the results which are expected in another two years.
“Breast hardening or shrinkage has a heavy influence on a woman’s quality of life after breast therapy,” says Dr Harris. “Being able to recognise and alleviate these symptoms will make a huge difference to patients.”
Tracking radiotherapy
Beyond the QuaRTUS trial, Dr Harris is also addressing the problem of motion and organ movement when delivering radiotherapy. X-rays can be used to guide radiotherapy planning, but these are hard to take during treatment, often not showing soft tissue clearly, and also give the patient an extra dose of radiation.
By using 4D ultrasound to track radiotherapy, images can be taken in real time, and soft tissues can be visualised clearly while putting the patient at no extra risk. “We can process internal tissue movement in real time, so can adjust the radiotherapy accordingly,” explains Dr Harris. “We are now testing this in prostate and cervical cancer studies, but hope to include liver and paediatric cancer patients in the future.”
Much like bats navigating in the dark, ultrasound is now being used to help navigate the path of cancer treatment. However, this is just one side of ultrasound’s many facets — we are also using it to locate tumours and alleviate bone cancer pain — making it a growing and formidable force in cancer research.