Background
Radiotherapy has been instrumental in the treatment of cancer for more than 100 years. Treatment is delivered over several fractions to improve tumour control and minimise normal tissue complications. Radiotherapy treatments are planned using electron density information obtained from computed tomography (CT) images to deliver the prescribed dose to the tumour while minimising dose to normal tissue.
Imaging biomarkers that could assess and predict response to treatment are of particular interest, for example to identify resistant subvolumes of the tumour or early signs of side-effects of radiation. MR-guided radiotherapy on a hybrid MR-Linac system enables novel treatment workflows but requires imaging solutions that are different from diagnostic MRI. Our research focuses on two key applications: Functional MRI to assess and predict response to therapy and 4D MRI to manage motion.
Functional MRI
To assess response to treatment, techniques based on diffusion-weighted MRI are particularly promising due to their association with response-related metrics, such as cellularity and cell membrane permeability. Our research interest here is to minimise geometric distortions in diffusion-weighted MRI for use in daily adaptive MR-guided radiotherapy and to enable the simultaneous characterisation of perfusion and diffusion using flow-compensated intravoxel incoherent motion (IVIM) imaging.
In MR-guided radiotherapy with MeV photons, the formation of reactive oxygen species plays an important role in the DNA damage mechanisms and reduced oxygenation (hypoxia) in the tumour is associated with resistance to radiotherapy. We’re working on fast MR relaxometry techniques including MR fingerprinting to perform dynamic T2* and T1 measurements and plan to combine these with oxygen-enhanced MRI to detect tumour hypoxia.
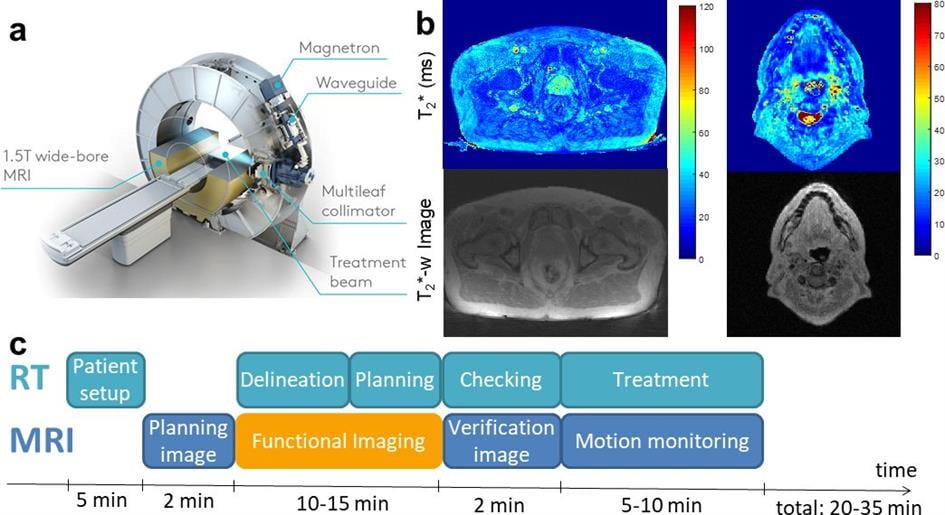
Image: a) Elekta Unity 1.5 T MR-Linac. b) T2*-weighted images acquired in patients treated for prostate (left) and head and neck cancer (right). c) MR-Linac Treatment workflow including daily functional MRI.
4D MRI
The excellent soft tissue contrast of MRI and the availability of MR imaging at the time of treatment minimises uncertainty about the position and extent of tumours and dose-sensitive organs-at-risk. This real-time information could be used to reduce the risk of radiation-induced side effects or to overcome resistance by boosting the dose to the tumour. Fully leveraging the potential of MR-guided radiotherapy requires replanning treatments using synthetic CT derived from MR images acquired a few minutes before treatment start. 4D MRI aims to characterise physiological motion including respiratory, cardiac and peristaltic motion to derive the correct treatment margins and to enable spatial mapping of the delivered radiation dose.
Following on from our previous work on 4D MRI for radiotherapy, we’re currently working on synthetic 4D-CT for the treatment of lung cancer patients. Together with Prof. Wayne Luk’s team at Imperial College London we are accelerating 4D MR image reconstruction and we are working towards volumetric real-time imaging on the MR-Linac system.
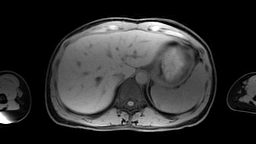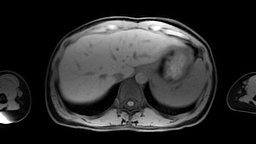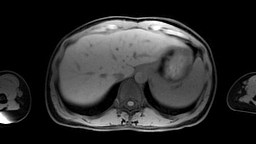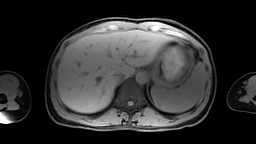
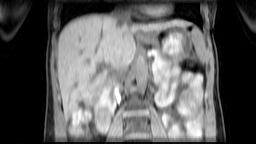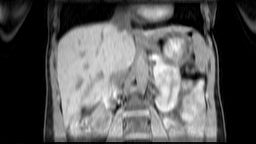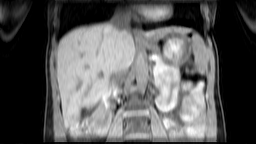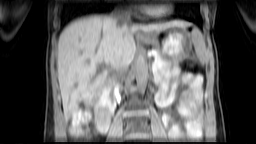
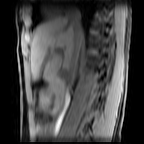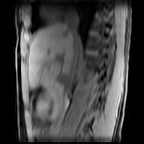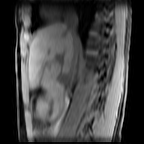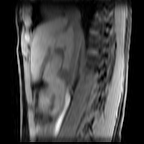
Images: Axial, coronal and sagittal views (left to right) of a 4D-MRI scan showing respiratory motion in the abdomen.