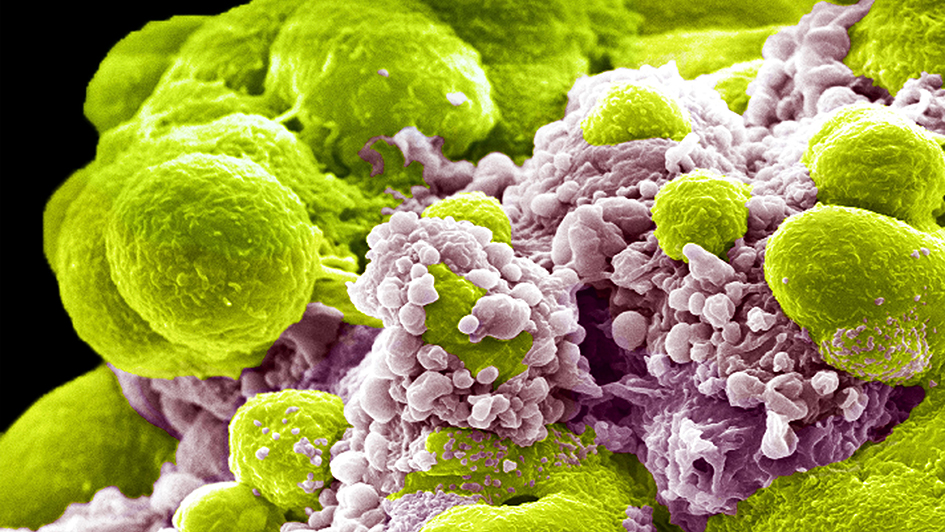
Image: Scanning electron micrograph of a multi-cellular prostate tumour spheroid (cluster of tumour cells) treated with nanomedicines carrying the anticancer drug doxorubicin. Credit: Khuloud T. Al-Jamal and Izzat Suffian. License: CC BY 4.0
Cutting-edge Big Data analysis used to find possible new drugs
Our scientists uncovered 80 potential lines of attack against prostate cancer.
In an important new study, researchers combined detailed genetic analysis with the latest Big Data approaches to identify large numbers of genetic changes that underlie the development and spread of prostate cancer. They then took this genetic information and drew up a map of the network of associated proteins.
Using canSAR, a comprehensive database for cancer drug discovery (led by Professor Bissan Al-Lazikani), an international team led by ICR scientists, found that 80 of the proteins in the network were possible drug targets.
Study co-author Professor Paul Workman, Chief Executive of The Institute of Cancer Research, London, said:
“We hope our findings will stimulate a wave of new research into the genetic changes and potential drug targets we have identified, with the aim that patients should benefit as soon as possible.”
Immunotherapy can benefit a subset of men
During last year’s American Society of Clinical Oncology annual meeting (ASCO) in Chicago, we published the news that a major trial was the first to show benefits of immunotherapy in some men with prostate cancer.
Researchers, led by Professor Johann De Bono, showed that a subset of men who had run out of all existing treatment options survived much longer than expected when taking the immunotherapy pembrolizumab.
The research also revealed vital clues for how to pick out the subset of men who could benefit.
Michael English, 72, was treated at The Royal Marsden, our hospital partner, in 2016. He said:
“Professor de Bono recommended pembrolizumab based on a genetic test and after only a few three-weekly cycles, when scans showed that the tumour had become undetectable.
“Personalising my treatment in this way, based on the genetic make-up of the tumour, essentially saved my life. With a fourth grandchild on the way, my wife and I can now plan for the next 20 years, instead of the next two.”
DNA test identifies men with six-fold increased risk of prostate cancer
We also released news about a new study of more than 140,000 men that had identified 63 new genetic variations in the DNA code, each of which increase the risk of prostate cancer.
Professor Ros Eeles, Professor of Oncogenetics at the ICR, said:
“By looking at the DNA code of tens of thousands of men in more depth than ever before, we have uncovered vital new information about the genetic factors that can predispose someone to prostate cancer, and, crucially, we have shown that information from more than 150 genetic variants can now be combined to provide a readout of a man’s inherited risk of prostate cancer.
“If we can tell from testing DNA how likely it is that a man will develop prostate cancer, the next step is to see if we can use that information to help prevent the disease.”
Researchers 'dreamed' of using MR Linac treatment
We were delighted to announce that the ICR and The Royal Marsden had delivered the first ever treatment in the UK to a patient using a Magnetic Resonance Linear Accelerator (MR Linac) machine.
The prostate cancer patient received radiotherapy treatment on the MR Linac as part of the PRISM clinical trial, which is the first of its kind in the UK.
The MR Linac combines cutting-edge radiotherapy technology with precision MR imaging capabilities, which will mean radiotherapy can be delivered more accurately than before because clinicians will be able to see where they are targeting in real-time.
Professor Uwe Oelfke, Head of the Joint Department of Physics at the ICR and The Royal Marsden, who leads the joint MR Linac project, said:
“For decades the radiation oncology community has dreamed of the day when we could see what we treat in real time just as our surgical colleagues do, and we are excited that this day has arrived.
“The ICR and The Royal Marsden have made world-leading advances in radiotherapy through our research and we expect the MR Linac to allow us to make another step change in improving cancer treatment.”
Better treatment by high-tech scans
Last year we also called for hospitals to use high-tech scans to diagnose prostate cancers when they can still be cured, following a new study.
The study found evidence that modern imaging tools such as PET and MRI were better than standard CT scans at telling apart cancers that had spread to a limited number of sites from those that had spread more widely.
Professor Nandita deSouza, Professor of Translational Imaging at the ICR, said:
“Our study found that modern scanning technologies hold enormous promise for more accurately picking out men with prostate cancer that has a limited spread.
“Men with prostate cancer deserve the best available technology to be brought into the clinic, so that those with a limited spread of disease can be offered the best possible treatment, and be given the highest chance of a cure while avoiding, where possible, toxic side-effects.”
A new approach to tackling cancer drug resistance
Another major study showed that a cancer-driving protein is found more in advanced prostate cancer, after hormone therapies, than in early-stage disease – and could therefore play a role in making the cancer resistant to treatment.
The research, led by scientists at the ICR in collaboration with US researchers, also suggested that researchers should look for new treatments that target this protein – called AR-V7 – and stop it from working.
Leader of the study in the UK, Professor Johann de Bono, said:
“This is the biggest study to date of AR-V7 protein expression in tissue biopsies from men with early and advanced prostate cancer, and shows that the emergence of the AR-V7 protein in cells is an important event in the development of resistance to hormone therapies like abiraterone, which was discovered at the ICR.
“If novel therapeutic strategies could prevent AR-V7 expression during hormone therapy, it could improve outcomes for men with lethal prostate cancer.”
Supporting our vital cancer research
Research at the ICR is underpinned by generous contributions from our supporters.
You can contribute to our mission to make the discoveries to defeat cancer.


