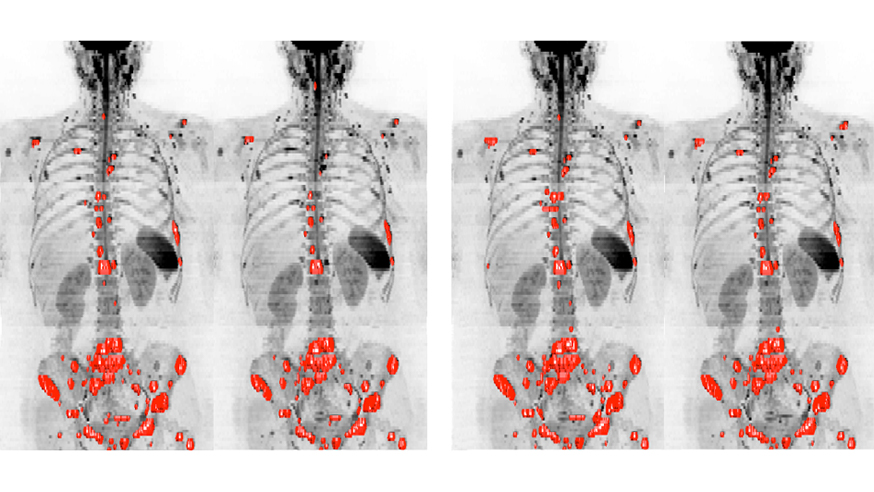
Image: Whole body MRI scans of a breast cancer patient, assessed by two observers, to measure tumours in the patient’s bones. The software could help clinicians reliably assess how bone disease changes over time (Credit: Blackledge et al 2016)
Modern, sophisticated scans should be used in hospitals to pick out men whose prostate cancers have only spread to a limited number of sites, so they can be offered the chance of cure, a new assessment concludes.
Researchers found evidence that modern imaging tools such as PET and MRI were better than standard CT scans at telling apart cancers that had spread to a limited number of sites from those that had spread more widely.
Using these modern scans could give some men the option of treatment focused specifically on the sites of spread – giving them a better chance of survival and potentially sparing them the side-effects of treatments that affect the whole body.
Experts at The Institute of Cancer Research, London, co-led an international team of cancer imaging specialists with the University of Louvain in Belgium, looking at the evidence on the possible benefit of high-tech scanning techniques.
The study is published in the journal The Lancet Oncology, and received support from Cancer Research UK and the Belgian charity Fonds Cancer.
The ICR's Magnetic Resonance team develops and tests new probes, instrumentation and techniques to better plan and assess cancer treatment.
Better treatment by high-tech scans
High-tech scans offer more sophisticated information about tumours, detecting them by their high rate of cell growth, the way they burn energy and the presence of certain receptors on cancer cells.
The new assessment of evidence found that this information improved the chances of distinguishing patients with only limited spread from those with more advanced disease, who cannot hope to be cured.
For example, a study involving 130 men with newly diagnosed prostate cancer compared a type of PET scan, in which a radioactive substance helps visualise prostate cancer cells while ignoring healthy ones, with standard CT scans.
The study found that the PET scan was better at detecting prostate cancer that had spread to bones or lymph nodes – detecting metastases with 89 per cent accuracy compared with 72 per cent using CT scans.
A pilot study involving 21 men found early evidence that whole-body MRI scans were able to measure the response of prostate cancer that had spread to a targeted drug, called olaparib.
Next: clinical trials
Having established the value of modern scanning technologies, the researchers are now planning clinical trials to study how these technologies can be used to inform and adapt the treatment plan for men whose prostate cancer is found to have spread to a limited number of sites.
For example, they plan to test whether offering men localised treatment – surgery or radiotherapy – when high-tech scans show they have advanced prostate cancer with limited spread could extend the time they survive without the disease coming back.
Another clinical trial will test whether men picked out using modern imaging tools could benefit from a short course of a drug called abiraterone which was discovered at The Institute of Cancer Research (ICR), when given alongside localised treatment to the sites to which their prostate cancer has spread.
Steve Cleary from Croydon has undergone regular scans for his prostate cancer as part of an ‘active surveillance’ scanning programme to monitor cancers which have not spread beyond the prostate. He reflects on the importance of having repeated scans:
"My third MRI scan after diagnosis picked up a small area that appeared to have become more aggressive. We knew then that I needed to proceed to active treatment. I have now been cancer free 18 months”.
'Enormous promise'
Professor Nandita deSouza, Professor of Translational Imaging at The Institute of Cancer Research, London, said:
“CT and bone scans are still the accepted way of diagnosing prostate cancer that has spread, but we found good evidence that other imaging technologies could do a better job.
“Our study found that modern scanning technologies hold enormous promise for more accurately picking out men with prostate cancer that has a limited spread.
“Men with prostate cancer deserve the best available technology to be brought into the clinic, so that those with a limited spread of disease can be offered the best possible treatment, and be given the highest chance of a cure while avoiding, where possible, toxic side-effects.”
Professor Paul Workman, Chief Executive of The Institute of Cancer Research, London, said:
“Cancer imaging has been transformed in recent years – modern, sophisticated tools such as PET scans can unlock a wealth of information about tumours that could be used to diagnose, monitor and treat patients more effectively.
“This new assessment of evidence suggests that modern types of scan could allow doctors to identify metastases earlier and more precisely, increasing the chances of successful treatment.
“I am keen to see evidence-based use of these scans on the NHS as soon as possible, so that more patients can benefit from the advances we have seen in imaging technologies.”