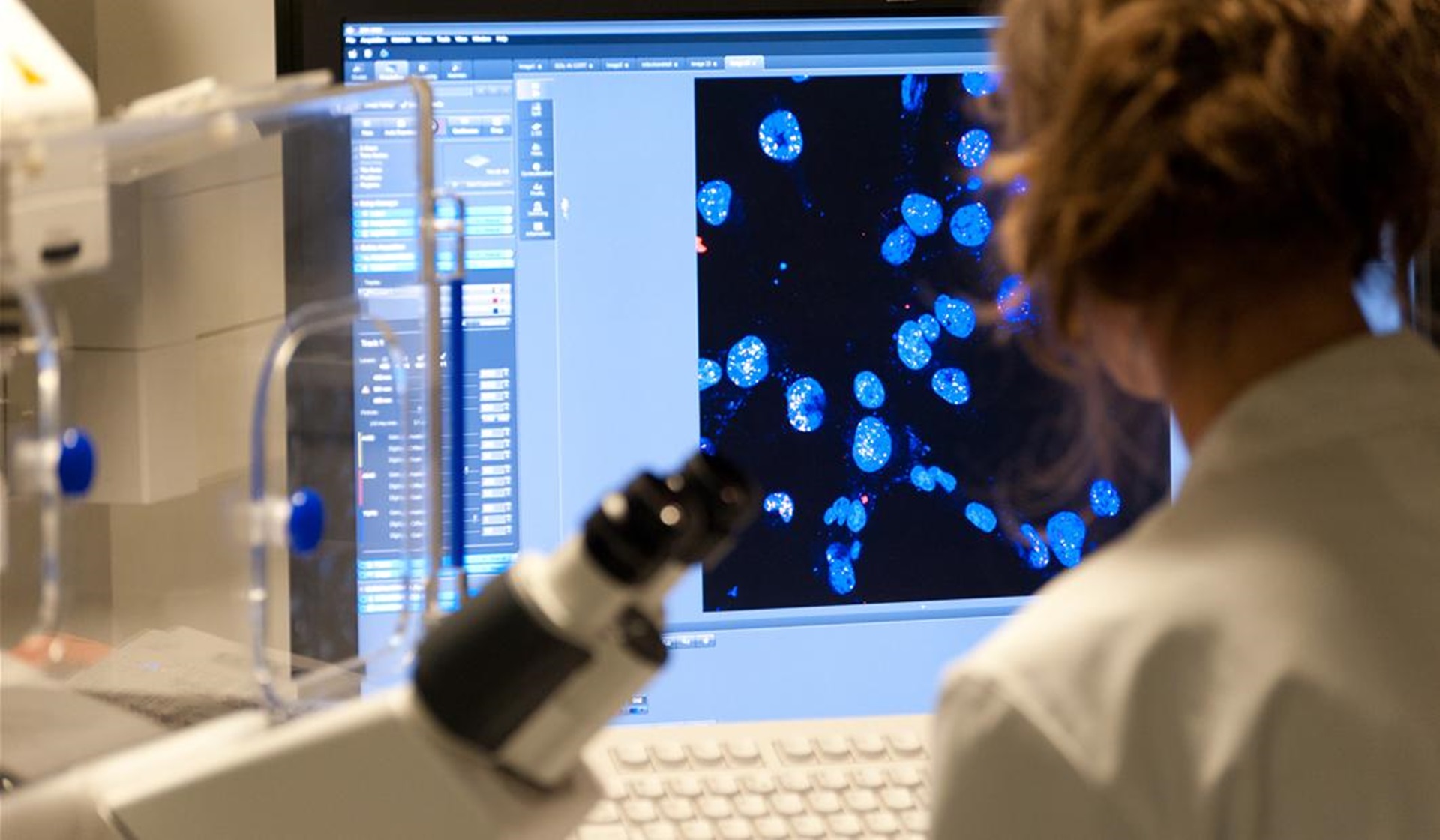
A new immunotherapy drug has shown promise for safely treating prostate cancer, a phase I trial reports.
Almost half of the patients in the trial that could be evaluated saw their tumour shrink after taking the drug, and the majority of patients experienced a marker of prostate cancer halved. The researchers were pleased to see that the majority of patients only experienced very mild side effects.
The phase I trial involved 8 sites around the world and is led by Professor Johann de Bono at The Institute of Cancer Research, London and The Royal Marsden NHS Foundation Trust.
T cell engager
Results from the trial, which was funded by Vir Biotechnology, are presented at the American Society of Clinical Oncology (ASCO) Genitourinary Cancers Symposium.
The trial tested the new VIR-5500 drug in 58 patients with advanced prostate cancer that has stopped responding to other treatments. The aim of the trial was to determine the safety of the drug and find the best dose to give to patients.
The innovative drug is a T-cell engager – it binds both to the body’s immune T-cells, and to prostate-specific membrane antigen (PSMA), which is on the surface of cancer cells.
Cloaking device
It binds to the cancer cells wherever they are in the body and brings the T-cells into contact with them, facilitating their attack. It also contains a cloaking device – keeping it hidden and inactive until it reaches the tumour – which helps to prevent side-effects from occurring. In addition, it allows the drug to stay in the blood stream for longer, meaning fewer doses may need to be given to patients.
T-cell engagers have previously led to severe inflammatory responses in prostate cancer patients, as they activate the immune system all around the body. Thanks to the cloaking device, 88 per cent of the patients did not experience the treatment-related adverse events usually seen with T-cell engagers.
Prostate-specific antigen (PSA) is a marker of disease that can be elevated if someone has prostate cancer. Of the 17 evaluable patients treated with the highest dose of VIR-5500, 82 per cent (14 patients) saw their PSA levels halved, and 53 per cent (nine patients) saw their PSA levels drop by 90 per cent.
Shrinks tumours
Of the 11 patients treated at the highest dose who could be evaluated, 45 per cent (five patients) experienced their tumour shrink after treatment. Scans showed that tumours had shrunk in multiple sites across the body, including the internal organs.
It is estimated that more than three quarters of the 10,000 men a year diagnosed with advanced prostate cancer have tumours with high levels of PSMA and could therefore benefit from the treatment.
'The kiss of death'
Professor Johann de Bono, Regius Professor of Cancer Research at The Institute of Cancer Research, London, and Consultant Medical Oncologist at The Royal Marsden NHS Foundation Trust, said:
“T-cell engagers empower the body’s own immune system to give cancer cells the kiss of death. It is really remarkable to see early signs that this T-cell engager drug can have a profound anti-cancer effect for patients with advanced prostate cancer, who desperately need new treatments.
“It’s very positive to see that very few patients have experienced major side-effects, as this has been a key challenge in treating prostate cancers with immunotherapies in the past.
“This clinical trial is ongoing, and the drug will now progress into larger trials so that we can study its effect on patients’ long-term outcomes. There is certainly hope that drugs such as this will increase the likelihood of a cure even from advanced prostate cancer that has already spread, in the not-too-distant future.”
Professor Kristian Helin, Chief Executive of The Institute of Cancer Research, London, said:
“Immunotherapy has transformed the outcomes for many people with cancer but for those with prostate cancer its benefits have often remained out of reach. It’s encouraging to see this innovative approach showing promising effects in early clinical studies, and I look forward to following its continued development. I hope that VIR-5500 may offer a new treatment option for patients with advanced prostate cancer, who urgently need more effective therapies.”





.tmb-propic-md.jpg?Culture=en&sfvrsn=c25d2b2f_9)