
Image: Andrew Wicks in the lab at The Institute of Cancer Research. Credit: Andrew Wicks.
I still remember getting my diagnosis, even though it was all a bit of a whirlwind. Within a couple of days, I’d gone from having a cough to having cancer. These things come at you fast!
At 12, I was very active and loved sports. That summer, I spent most of my time playing football or rugby, or doing athletics at school. I developed a persistent cough, but because I seemed so well otherwise, my family and I didn’t think much of it. When the antibiotics the doctors had given me didn’t work and I was sent to the local hospital for a chest X-ray, we assumed an infection was to blame.
Instead, the X-ray revealed a visible tumour the size of an orange in the lymph nodes around my lungs. Suspecting lymphoma, the doctors put me in an ambulance and sent me to Great Ormond Street Hospital, a children’s hospital in London. There, I had a bone marrow biopsy, which showed that I actually had acute lymphoblastic leukaemia (ALL).
ALL is a type of blood cancer that results from the bone marrow making too many immature white blood cells called lymphocytes. Many of the initial symptoms, including fatigue, frequent infections, and a fever, are nonspecific, but it’s important to start treatment immediately. Without treatment, the disease progresses very quickly and is fatal.
I didn’t really digest the news at first. I was too numb, too shocked to be scared. I just went into autopilot and tried to adapt to the situation as it rapidly changed. However, I vividly remember my parents being scared and upset. They were devastated by my diagnosis.
Luckily, because leukaemia is the most common type of cancer in children, and ALL is the most common type of leukaemia at this age, doctors know how to treat it.

Image: Andrew aged 12, before receiving the ALL diagnosis. Credit: Andrew Wicks.
I can now reflect on how tough the treatment was
I started on high-dose chemotherapy, which was very intense. It made me feel nauseated and fatigued, and it weakened my immune system. For a year, long hospital stays and my low immunity meant that I was unable to go to school or anywhere else really. Most of the time, I felt too poorly to leave the house anyway. But I missed seeing my friends, having a social life and playing sports. My mum stopped working so that she could stay at home with me and take care of me, and my dad took a lot of time out from work so that he could be at my hospital visits.
My trips out were mainly to the hospital, which I visited at least once a week. I underwent procedures such as bone marrow biopsies and lumbar punctures, and I received chemotherapy as an outpatient there. Now, as an adult, I can reflect on how tough the treatment was, but at the time, I tried to keep a positive mindset, focusing on taking each day at a time and getting through it. To me, each treatment or hospital visit meant that I was taking a step closer to the finish.
Once I moved onto maintenance therapy, I was able to return to school, and my mum went back to work. The side effects of the treatment were more manageable, and my life started to feel a bit closer to normal. I was able to see my friends again and to go into town. But then, in the third year of my treatment, my ALL relapsed. I felt very dispirited because treatment had been going so well, but my doctors still had hope.
I needed to try a new form of treatment, so they recommended that I undergo a stem cell transplant. I had to have high-dose chemotherapy and radiotherapy to deplete my immune system before the transplant. Then I had to take immunosuppressive drugs to prevent my immune system from rejecting the donor cells and to prevent the donor cells from attacking healthy cells in my body.
Again, I had to be really careful to protect myself from infection while my immunity was low. I ended up taking some of my GCSE exams while in hospital for treatment because I was stubbornly determined not to let it disrupt the normality that had seemed so close. But it felt like a step backwards.
That’s why, when I had finally the long-desired appointment in which they told me that I was done with treatment and would only need to see the team again for checkups, my first feeling was just incredible relief. “We’re here,” I remember thinking. “We’ve made it!” It was such a happy moment for my family. My parents, two brothers and sister had all gone through it too. My diagnosis and treatment were tough for everyone.
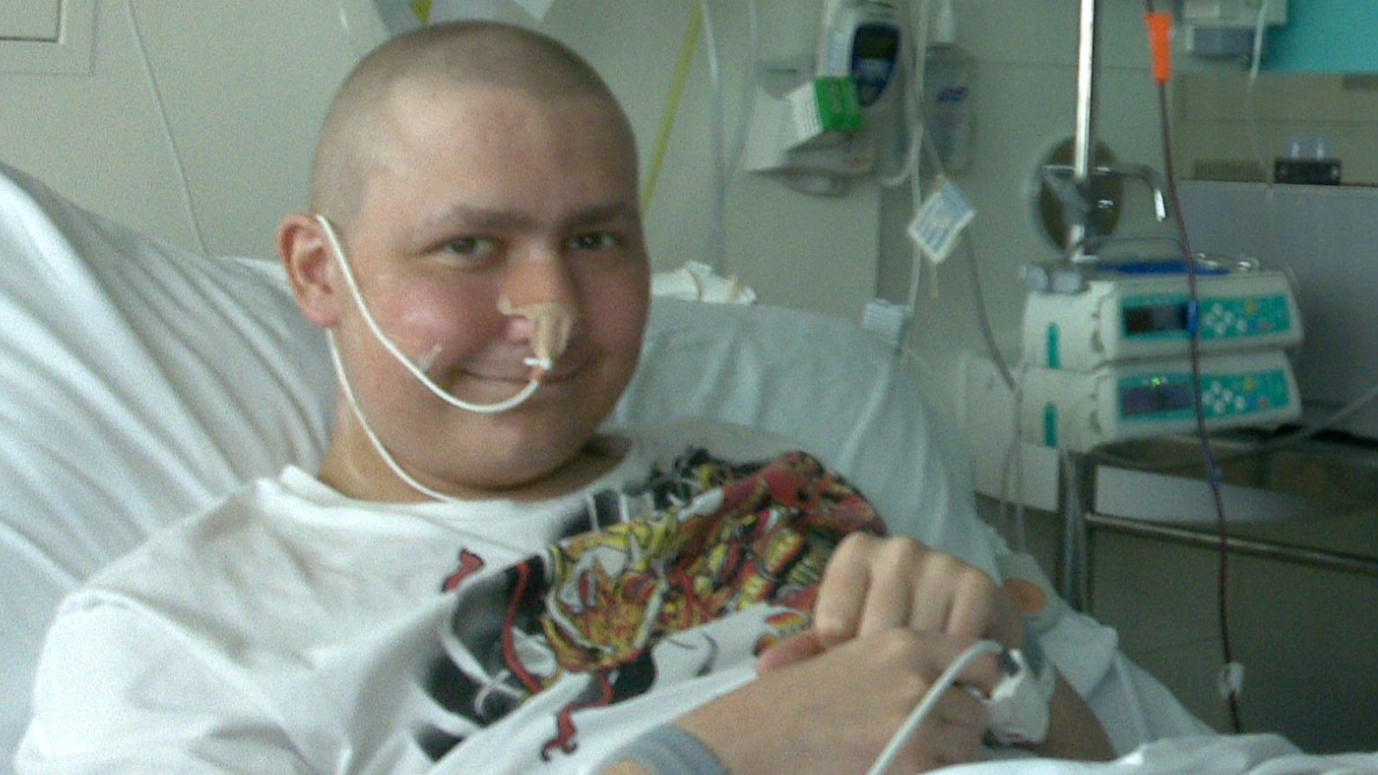
Image: Andrew receiving stem cells in the hospital. Credit: Andrew Wicks.
I was interested in how research leads to new treatments
The support and care I received from hospital staff and my family were incredible, and I can’t express enough how much that helped me.
With hindsight, I was probably quite an annoying patient! Seeing lots of other people with cancer and hearing about many different treatments meant that I always had lots of questions. “What is this drug?” I would ask. “How does it work?” I took part in clinical trials during my treatment and, even as a young patient, I was intrigued by how research leads to new treatments.
Three years after completing treatment, I chose to study biology as an undergraduate. Learning about cancer in detail – the different types of the disease and how it develops and progresses – furthered my interest, and I went on to complete a Master’s degree focused on cancer drug resistance. Wanting to get some research experience and learn even more about cancer, I joined The Institute of Cancer Research, London, as a Scientific Officer (technician) in Professor Chris Lord’s lab in the Division of Breast Cancer Research.
I learned a lot during this time from my colleagues, who are among the leaders in their field. I knew that, given the expertise and breadth of knowledge in the team, there would be nowhere better for me to learn and undertake my own independent research project.
I am now in the fourth year of my PhD here at The Institute of Cancer Research (ICR). Supervised by Professor Lord and Professor Andrew Tutt, Head of the Division of Breast Cancer Research and Director of the Breast Cancer Now Toby Robins Research Centre at theICR, I am working on a project investigating PARP inhibitors. In particular, I am studying how tumour cells ‘react’ and change when exposed to these agents, and how these changes might confer drug resistance. The long-term aim is being able to prevent or treat this resistant disease.
Support for leukaemia research at the ICR
This year’s ICR Christmas fundraising appeal features the story of Tommy Edwards, a seven-year-old who is currently responding well to treatment for ALL, the same type of cancer I had.
Tommy’s parents, Jo and Chris Edwards, have set up a charity called Prevent ALL, which is funding work by the highly-honoured Professor Sir Mel Greaves, Founding Director of the ICR’s Centre for Evolution and Cancer. Professor Greaves’ research shows that leukaemia, including ALL, may be preventable, and his team is working towards developing simple and safe interventions to stop the disease from developing.
All of us at the ICR are incredibly grateful for the support we receive from our amazing family charity partners like Prevent ALL. Without them, a lot of the work we do would not be possible.
Cancer is hard for everyone, including family members. In my experience, it’s important, where possible, to have moments where the focus on the disease is temporarily put to the side and you are just a family, as you were before the diagnosis. I hope that Tommy and his family have the opportunity to do just that this Christmas.
We are world-leaders in the study of cancer in children, teenagers and young adults and have made huge strides over the past decade in understanding the causes and improving treatments. With your support, we can make the hope of safer, kinder and more effective treatments a reality for these children. Help cure more children with cancer, more kindly.
Image: Tommy Edwards. Credit: ICR/John Angerson.
The important thing is that we keep going
We still have much to learn about childhood cancer, but it is clearly not the same as adult cancer. Ideally, we should be treating it accordingly. We need treatments that are targeted to children and more appropriate for their needs.
Although the priority is, rightly, to provide treatments that are as effective as possible, in an ideal world, they would be much kinder too.
While I feel exceedingly fortunate that my treatment was successful, the debilitating side effects cost me at least a year of my childhood. Kinder treatments could allow children to go to school, see their friends and generally have a life outside of their illness. I believe that improving the quality of life for children with cancer is nothing short of essential.
At the ICR, I’ve seen with my own eyes the strong connection between work in the labs and the resulting benefits for patients. The translational aspect of the ICR’s work means that it has a direct impact on people. I find it very motivating to work at an institution that is so well-placed to change clinical practice for the better.
Although I don’t work in the field of paediatric cancer, when I think back to my childhood, it makes me feel really positive about my career choice. Knowing that my current research might go on to help others who find themselves facing a cancer diagnosis means that I look forward to Monday mornings.
I’m hopeful that, one day, outcomes can be improved for everyone living with cancer, and I’m proud to be contributing to this mission. The important thing is that we keep going.

