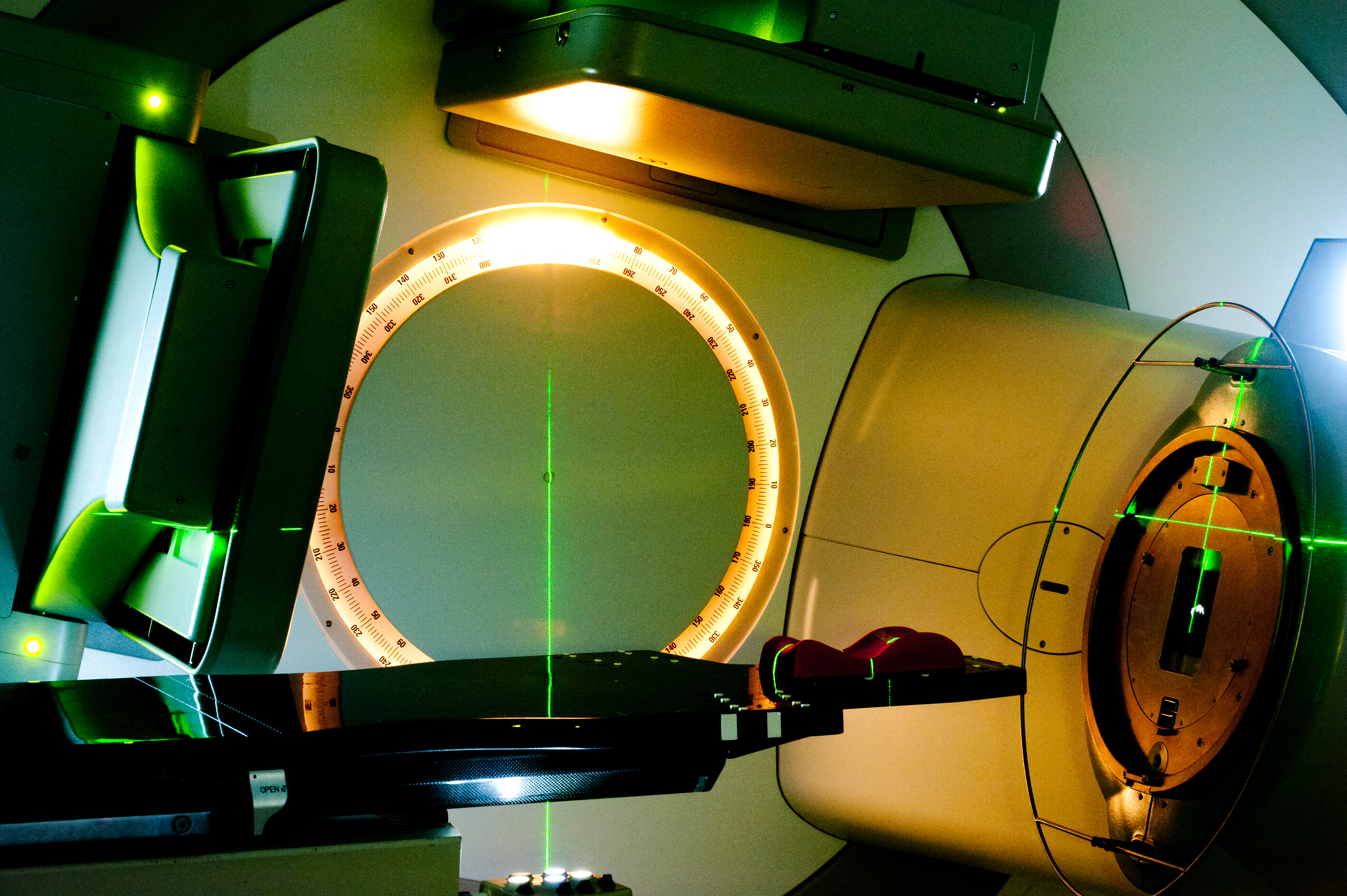
Since the discovery of X-rays in 1895, radiation therapy, or radiotherapy, has made substantial advancements as a cancer treatment. It’s now responsible for approximately 40 per cent of cancer cures. Yet access to radiotherapy could be threatened by the predicted increase of cancer incidence and the growing pressure healthcare systems already face.
Research to make radiotherapy treatment faster and more accurate could be the solution. Scientists at The Institute of Cancer Research, London, and clinical colleagues at The Royal Marsden NHS Foundation Trust, are particularly focused on how the imaging techniques that guide radiotherapy could be delivered in a way that ensures the latest and most innovative radiotherapy treatments are widely available for the growing numbers of cancer patients.
Transforming how radiotherapy is delivered
Modern radiotherapy relies on treatment integrated imaging (magnetic resonance imaging (MRI) and computed tomography) to allow clinicians to pinpoint tumour boundaries and nearby tissue, so that the optimal dose can be carefully designed to maximise the delivery of targeted radiation to the tumour and minimise the levels of radiation that affect healthy tissue.
Real-time MRI of the patient provides one of the foundations for adaptive radiotherapy which allows for treatment plans to be tweaked based on natural anatomical changes during treatment, such as a patient’s breathing pattern or bowel movements.
This approach is made possible by advanced technologies such as the MR Linac – which combines an MRI scanner and a radiotherapy linear accelerator to precisely locate tumours and accurately deliver doses of radiation to moving tumours.
The Institute of Cancer Research (ICR) in partnership with The Royal Marsden is seen as a leader in developing emerging radiotherapy techniques for use in clinical settings. Alongside the MR Linac, we are pioneering ways for radiotherapy to be delivered in in higher doses over fewer sessions, without compromising on the quality of treatments. Our dedication to radiation-related research, working in close partnership with colleagues at The Royal Marsden, was recently recognised with a Queen Elizabeth Prize for Higher and Further Education.
A catalyst for change

Professor Uwe Oelfke, Head of the Joint Department of Physics at the ICR and Professor Anna Kirby of The Royal Marsden, have secured new funding from Cancer Research UK (CRUK) to advance the development of clever radiotherapy techniques that will help us keep ahead of any rise in cancer cases.
Professor Oelfke said: “Adaptive radiotherapy has great potential to improve how we treat many cancer types, but the current workflows can be time-intensive and technically demanding. The outcomes of our new CRUK-funded programme will overcome these hurdles by developing automated technology and leveraging artificial intelligence (AI) to make adaptive radiotherapy faster, easier to execute and more accessible.”
The £2.5 million Discovery Research Programme grant will support research, over five years, into automated high-precision AI accelerated radiotherapy. Professor Oelfke will lead the research in close collaboration with clinical teams at The Royal Marsden, led by Professor Anna Kirby. The research team aims to transform how radiotherapy is planned and delivered and greatly improve the experience for patients.
Professor Kirby, a Consultant Clinical Oncologist at The Royal Marsden, and Professor in Radiotherapy for Breast Cancer at the ICR, said: “Our new CRUK-funded programme of work will better support healthcare professionals in delivering the most targeted radiotherapy in the most efficient way, optimising outcomes for our patients as well as improving patient experience.”
Accelerating innovation using AI
The research programme will be split across four streams of work:
- Facilitating real-time therapy adaption
- Accelerating online adaptive radiotherapy workflows
- Advancing MRI-guided radiotherapy technologies
- Demonstrating the clinical benefit through patient studies
The team will develop AI systems to rapidly analyse MRI images and predict anatomical movement during treatment. These tools will enable clinicians to adapt radiotherapy in real time as needed, ensuring it remains highly targeted to the tumour. The programme team will also develop advanced quality assurance systems to monitor treatment as its delivered, ensuring it is administered safely.
They aim to reduce preparation time and cut workflows by 50 per cent by combining deep learning – an AI subtype using artificial neural networks to simulate the human brain's decision-making process - automated image segmentation and instantaneous treatment planning.
The team will also explore the use of generative AI tools – such as voice recognition and eye-tracking technology – to support the review of patient profiles and treatment decisions. The research could lead to adaptive radiotherapy planning being completed in less than 15 minutes for cancers such as pelvic, lung and head and neck, without compromising the quality of care.
Professor Oelfke and the team will also expand the use of existing MRI-guided radiotherapy systems – such as the MR Linac. The Royal Marsden, working in partnership with the ICR, was the first cancer centre in the UK to have this specialist system installed. The installation of the MR Linac was made possible by a £10m grant from the Medical Research Council (MRC) to the ICR, with additional support from The Royal Marsden Cancer Charity.
However, the MR-Linac isn’t widely available across the NHS, so the team will therefore investigate a new hybrid treatment pathway using less advanced and more cost-effective MRI scanners to guide radiotherapy before it is delivered on conventional machinery.
Will these innovations make a difference for patients? The researchers will answer this question via clinical studies performed at The Royal Marsden. These studies will evaluate whether the new approaches can safely enable emerging radiotherapy techniques such as ultra-hypofractionated radiotherapy – which delivers higher doses over shorter time periods, while maintaining and improving the effectiveness of treatment.
Leadership in radiotherapy
Professor Oelke, who is also Deputy Head of the Division of Radiotherapy and Imaging at the ICR, is an internationally recognised expert in adaptive radiotherapy. He previously developed one of the first systems capable of compensating for anatomical shifts during treatment, enabling clinicians to track tumours and adapt radiation delivery as required.
Professor Kirby has led international clinical trials in breast cancer radiotherapy working in collaboration with the ICR’s Clinical Trials and Statistics Unit over the past 15 years. Her work in reshaping treatment schedules and evaluating new technical approaches has helped to optimise the balance between treatment effectiveness and the side effects felt by patients.
The five-year programme will draw upon decades of expertise across numerous multidisciplinary teams in medical physics, imaging, computer science, radiography and clinical oncology at the ICR and The Royal Marsden.
The teams will also collaborate with University College London (UCL) Hawkes Institute and the UCL Medical Physics and Bioengineering Department, as well as industry partners, such as the radiation therapy manufacturer Elekta, Accurray, Siemens and the radiotherapy software developer RaySearch. These existing relationships will support the eventual translation of the programme into clinical practice, reaching patients worldwide.
The next five years
By combining cutting-edge methods with clinical insight, the team hopes to deliver a new generation of efficient and more accurate radiotherapy treatments, capable of meeting the growing demand for cancer care and delivering improved benefit for patients.
Professor Kirby said: “We are delighted that CRUK continues to recognise and support the strength of the historic partnership between the ICR and The Royal Marsden, where we have the opportunity to translate new methods rapidly and effectively, directly into clinical practice. The grant comes at a vital time and lays the foundation to deliver smarter and more effective treatments to meet the growing global need for efficient cancer care.”
Professor Oelfke said: “It is likely we will see a rise in cancer incidence, so we must prepare ourselves in finding new ways to deliver effective treatment strategies at scale. The ICR, together with The Royal Marsden, is well positioned to support this and with the new grant we can advance radiotherapy to benefit even more patients as the future unfolds.”