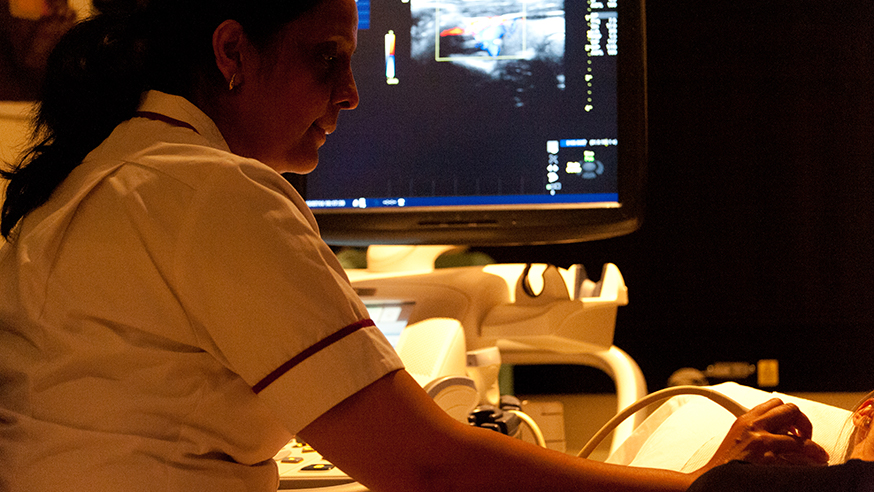
An ultrasound examination (photo: Jan Chlebik/the ICR)
Ultrasound is found in hospitals and doctors’ surgeries all over the world, and many of us will have been scanned at some point in our lives, even if it was before we were born.
At its simplest, medical ultrasound uses high-frequency sound waves to create images of areas inside of the body. Now, more sophisticated applications are being tested in cancer.
During the course of their treatment, nearly half of all cancer patients receive radiotherapy, which directs high-energy beams of radiation at tumours inside the body to destroy cancer cells.
Radiotherapy is carefully planned to avoid damaging healthy tissue as much as possible, but tumours can move or change shape during treatment, so some damage to surrounding tissues is often inevitable.
We’ve talked about ultrasound in the past, discussing how high-intensity beams of ultrasound can be used to blast tumours as an exciting new way to treat cancer.
But ultrasound can also improve how we deliver and monitor radiotherapy by providing accurate measurements of the position of the tumour.
-590x332.jpg)
Detecting tissue movement using ultrasound (image: Dr Emma Harris, image from Emma Harris et al, Physics in Medicine and Biology 2016)
Dr Emma Harris is Leader of the Imaging for Radiotherapy Adaptation Team at The Institute of Cancer Research, London, and she’s involved with two clinical trials which are using ultrasound to monitor tumour motion in patients with cervical cancer and prostate cancer.
At the moment, we rely on markers implanted into the prostate to guide prostate therapy, but these markers cannot easily be used to monitor the motion of the prostate during treatment. For patients with cervical cancer, we use cone-beam CT, which does not always give us a good image of the cervix and uterus.
Controlling the 'shape' of radiation
Dr Harris is using ultrasound image guidance for patients with prostate cancer, to locate the prostate and monitor its position during radiotherapy. She’s comparing how ultrasound measures up to other techniques to see if it can improve radiotherapy.
She recently teamed up with Professor Uwe Oeflke’s lab, and together they were the first to demonstrate that ultrasound can be used to control machines used to deliver radiotherapy. These machines use multi-leaf collimators, which are adjustable metallic ‘leaves’ that control the shape of the radiation beam, and by adding feedback about prostate position from ultrasound, multi-leaf collimators can adjust the radiation beam to follow the motion of the prostate. They have shown that this can improve the accuracy with which radiotherapy is delivered.
And ultrasound may be able to do more than just help track cancer. Different tumours, or even, different regions within tumours can respond differently to radiation depending on their biology, and ultrasound may be able to pick out this variation to help doctors make better decisions about the best course of treatment for a patient.
Tracking treatment response
In a recent review paper, Dr Harris explored the potential of ultrasound to measure treatment response. For example, tumour hypoxia occurs when cancer cells are deprived of oxygen, and it’s known to lead to cells that are more resistant to radiotherapy. Dr Harris believes that ultrasound may be able to measure tumour response and identify these regions at early stages of therapy, which may improve outcomes for patients receiving radiotherapy.
Ultrasound has the advantage of being an affordable technology, which can be integrated with any standard radiotherapy treatment machine, allowing doctors to scan patients at multiple times during their therapy.
From planning radiotherapy and guiding treatment as it happens, to assessing how tumours respond to therapy, ultrasound is helping doctors see cancer in a whole new way.


