In April 2019, I went on a journey - not one I expected to go on or even particularly wanted to go on, despite being an enthusiastic traveller. But in life we are often taken down unexpected paths. I’m a committed mason of over 40 years and have always been very active in my lodges and province. When a local prostate cancer charity was chosen as the charity for the Masonic year, I went along to a screening session at a local Masonic centre.
I was 58 at the time and didn’t really think anything of it. I was quite fit and healthy, and certainly didn’t think I had any of the main symptoms of prostate cancer.
Then I received an e-mail with the results of a blood test that had been conducted to assess the levels of a protein called prostate specific antigen (PSA). They used a traffic light system to categorise the results, and my PSA result was red. My score was 299.4. For a man my age, it should have been 4.0 or below. I started shaking, almost going into shock. I read the e-mail again. ‘It must be a mistake’, I thought.
As advised in the e-mail, I immediately went, head spinning, to my GP surgery and managed to get an emergency appointment once I had told the receptionist my news.
“I’ll be ok,” I told myself, ‘the test is not fool proof, I’ve got no symptoms.” A sleepless night ensued - one of many.

“I was determined to be positive”
After seeing my GP, I was fast-tracked through to a urologist at Royal Hampshire County Hospital, Winchester. I was told I probably had prostate cancer, and I was then booked in for an MRI scan, a PET scan and biopsy.
I went to all my appointments with much trepidation and fear. But without fail, every single member of NHS staff I came into contact with was fantastic - compassionate, professional, knowledgeable, friendly, happy and empathetic. I cannot thank them enough for the way they looked after me and continue to do so.
I was eventually diagnosed with stage 4 aggressive advanced metastatic prostate cancer. My Gleason score was 4 + 4 = 8. Ten is the maximum score you can have.
I had taken a good friend along to the appointment for support and afterwards we went to have a beer. It was a chance for me to message my family and friends, to break this very difficult and painful news. It was devastating, but I was determined to be positive. ‘I’m still alive’, I thought. I was going to have treatment and tackle this unwanted ‘squatter’ face on, the best I could.
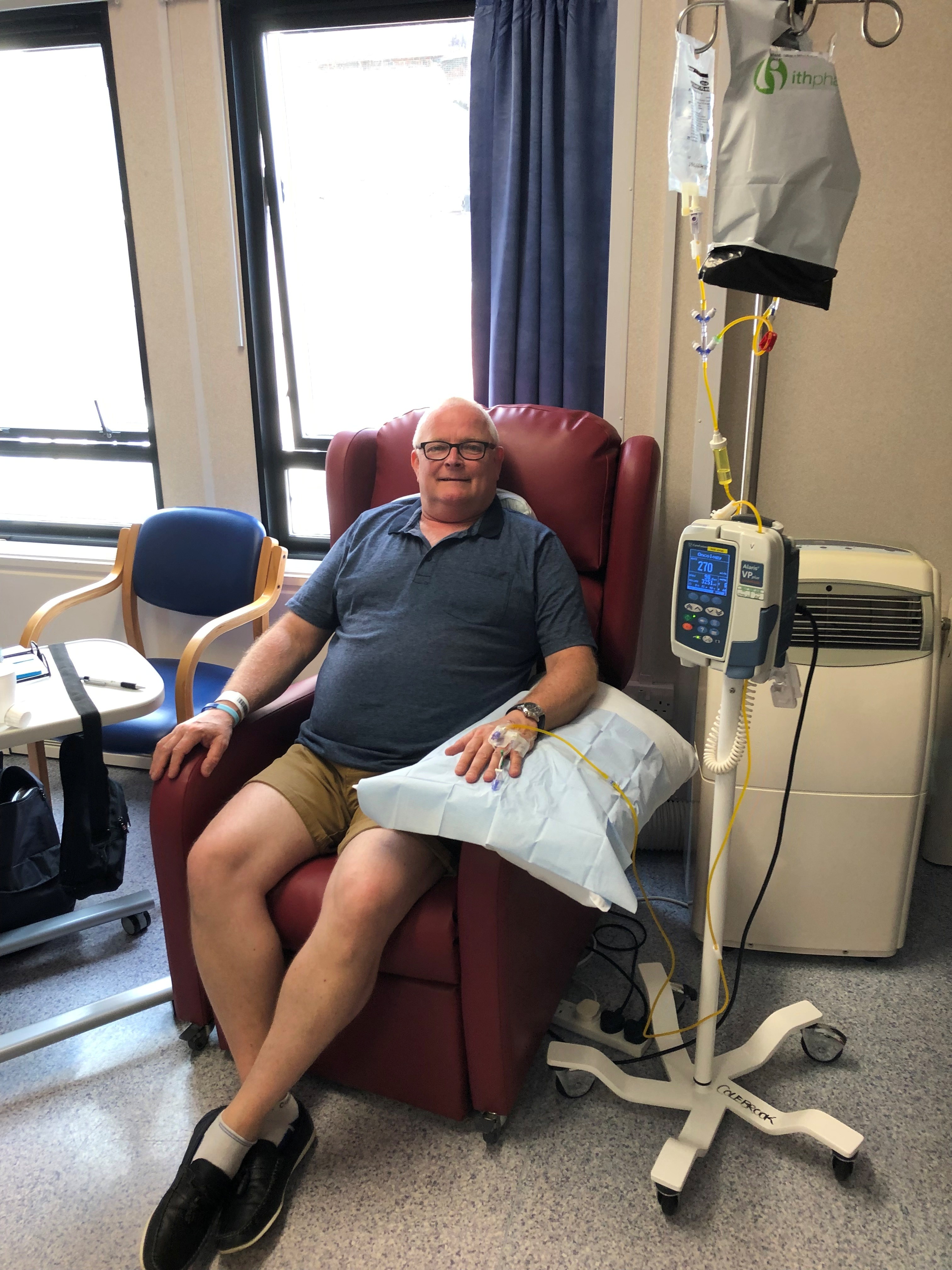
“My oncologist was very knowledgeable and empathetic”
It was hard telling people, but I received so much support from family, friends, former colleagues and lodge groups.
A few people said, “Oh, it’s only prostate cancer, you will be alright! They can sort that out…” All I could think was, ‘Maybe if it hadn’t spread…’
A few weeks after seeing my urologist, I received a letter to go and see my appointed oncologist – a lovely doctor, very knowledgeable and empathetic.
She explained a little more about my cancer, showed me my scans, explained where it had spread, told me of the support available to me and finally addressed a key question I had: life expectancy.
She told me, “On average you have a three-to-five-year survival rate.” - I still remember thinking, 'three to five years left with your family, your friends and loved ones! Just let that sink in!’
Had it been caught sooner, before it had escaped from my prostate, the prognosis would have been a lot better.
My oncologist said, “We cannot cure you, but we can control it, and we’ll throw the kitchen sink at it, due to your health and age.” Thankfully I was in good health and relatively young.
“I agreed to go on the STAMPEDE trial”
My initial treatment was hormone therapy that caused side effects like hot flushes, night sweats and weight gain. It also affected my libido and sexual function.
I agreed to go on the STAMPEDE trial, which aimed to investigate the best treatment for men with newly diagnosed advanced prostate cancer.
From 23 September 2019 I had a course of chemotherapy – docetaxel, every three weeks for six cycles, with my last one on 6 January 2020.
I then took a little break from the chemo to have 20 blasts of radiotherapy - one blast for 10 – 15 minutes every day except weekends.
The afternoon after my first chemo session, my trials nurse phoned to tell me that my PSA score from my recent blood tests was now 1.6, down from 299.4. It meant the hormone treatment was working, in just over two months.
I was also sent for a bone scan to check if the cancer had spread to my bones- luckily it hadn’t!
It was a trying time, but with the help and support of my family and friends, I got through it.
About three weeks after my last chemo session on 6 January 2020, I had a CT scan and was told the chemo had done what they had expected it to do! My PSA score was much lower and continued to drop.
For many years I had worked at as a Parks and Open Spaces Manager, and my former work team and friends sent me a rota they had compiled to take me to hospital in Basingstoke for my radiotherapy. It was lovely gesture and one I was very humbled and grateful for.
“My friends and neighbours helped me through lockdown”
Leading up to my last week of radiotherapy though, another dark and worrying cloud was looming over the horizon - Covid-19 was becoming more prevalent in the UK.
I was clinically vulnerable so had to self-isolate, but I continued to have phone consultations with my oncology team. They were pleased with my progress and my PSA continued to drop until it was undetectable.
My friends and neighbours were brilliant during lockdown, doing my shopping and ensuring I was ok, keeping me sane and having social distanced garden meets. One very close friend and I met every Sunday afternoon for drinks in the garden four metres away from each other!
As the world started to open up, I slowly began to do a little more – daily walks, socially-distanced walking meetings with my clients and going to see friends outdoors at home, restaurants and in their gardens.
Since then, my PSA readings have remained low. I continue with my hormone implants, blood tests and oncology consultations every three months.
I’ve always loved to travel and have an interest in both world wars. As a young man I worked for the Commonwealth War Graves commission in Passchendaele, Flanders and the Netherlands as a Head Gardener. In recent years, I have had some fantastic and memorable times in Scotland, Belgium, Germany, Holland, Menorca, Denmark to name but a few. After working for local authorities, I now work for myself as a consultant in parks, open spaces and land management.

“I was proud to have been on the STAMPEDE trial”
I want to talk about what happened to me because if I can save even one man from going through what I have, I will do anything I can.
The treatment is hard and unrelenting. I’ve learnt to live with the side effects of the ongoing hormone treatment that I’m having - for example, I have a hand fan and carry a small flannel to help with hot flushes. I have neuropathy in my feet so have found comfortable shoes that help with that. It’s about learning to adapt to my new life and make changes.
Further research is needed to find better ways to test for and treat prostate cancer. I was proud to have been on the STAMPEDE trial.
We also need more accurate and effective ways of diagnosing men at an early stage. I was adopted so I didn’t know whether there was any prostate cancer in my family.
“I’m determined to just live life to the full”
It’s been over six years since I was diagnosed – so I’ve now made it beyond the three to five year prognosis I was originally given. Going for that PSA test saved my life - the cancer hadn’t gone into my bones. If it had spread further, my prognosis could have been 12 months or even less.
Now when I’m asked about the cancer, I say, “It’s just sleeping.” Sometimes people say to me, “You must be pleased it’s gone”, and I think, “Errrr, no it hasn’t!” Because to me, it is just sleeping. And I hope it stays that way.
No one on this earth knows what’s round the corner. I’m keeping busy, still running my consultancy business, out most days for various Masonic meetings around the country and abroad, travelling, my usual trips to the Chelsea Flower Show, meeting friends, going to the theatre, having a few beers or wine and dining out, and of course spending precious time with my many friends and family. I am determined, to the bitter end, to just live life to the full - after all, life is for living.


