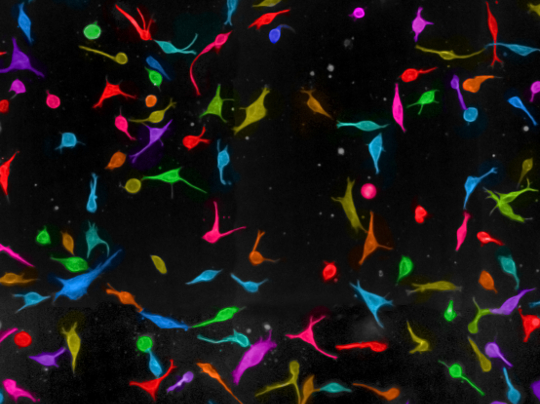
Skin cancer cells can change their shape and invade tissue via two separate routes, offering clues for how the disease is able to spread and become resistant to treatment, new research reveals.
For the first time, scientists have watched the cells of malignant melanoma – the most dangerous form of skin cancer – shift between forms that each have the ability to invade different tissue types.
Researchers at The Institute of Cancer Research, London, and Imperial College London grew and observed single melanoma cells in a 3D environment that closely resembled body tissue.
By using computational imaging techniques developed at the ICR, the team was able to watch these melanoma cells change shape over time.
The melanoma cells under observation were able to switch between the spindle-like ‘mesenchymal’ cells and the more rounded amoeboid cells in one of two ways – which researchers called the ‘polar’ and ‘apolar’ routes. The researchers also identified genes that cells need to take one route or another. The ability to shift between two cell shapes could help melanoma cells invade different tissues and potentially even to survive the effects of chemotherapy.
Senior author Dr Chris Bakal, who leads the Dynamical Cell Systems Team at the ICR, said: “We found that melanoma cells can change their shape in two ways – the polar and the apolar route. One implication of this is that if cells are trying to change shape to invade a particular type of tissue, but their route for doing so is blocked – by a drug for instance – there is another route, or ‘detour’ which the cells can use to change their shape and thus invade the tissue. Because we found genes controlling these shape changes, this study offers clues for designing new and more effective therapies that block the main route as well as the detour.”
Pioneering work at the ICR identified two distinct shapes which melanoma cells occupy during metastatic disease – rounded ‘amoeboid’ cells and spindle-shaped ‘mesenchymal’ cells. Following on from this, researchers elsewhere discovered that melanoma cells can change their shape from one form to another, but the mechanism by which cells do this was previously unknown.
In the paper published in Molecular Biology of the Cell, the scientists describe their use of a computational method of image analysis, the researchers were able to determine the shapes of melanoma cells in an unbiased manner. Image analysis by eye, although leading to useful scientific findings, is subjective as it relies on human judgment on the shape of cells. The computer program employed by researchers from the ICR and Imperial was not given instructions on what to look for and was instead designed to decide for itself which group of shapes a particular cell belonged to.
Speaking about this approach, Dr Chris Bakal said: “We wanted a computer to decide, in an unbiased way, what shapes melanoma cells are actually able to configure themselves to. We didn’t tell the computer beforehand what cell shapes should be present in the population of cells.”
Using their computational imaging tool, the researchers were able to identify additional shapes which melanoma cells can configure themselves to. The tool was also able to observe transitions between the two most abundant shapes – the mesenchymal and the amoeboid-type cells.
Dr Chris Bakal said: “We found that the two previously described cell shapes do exist, but additional cell shapes were present in the 3D environment used in our study.
“The differences in shape we saw in these melanoma cells – and indeed in other types of cancer – might be explained by the fact that these cells can take one of two routes to switching their shape. Now that we understand that these two routes exist, we might be able to design personalised treatment programmes for patients with metastatic melanoma by blocking the ability of cells to shape change via these routes.”