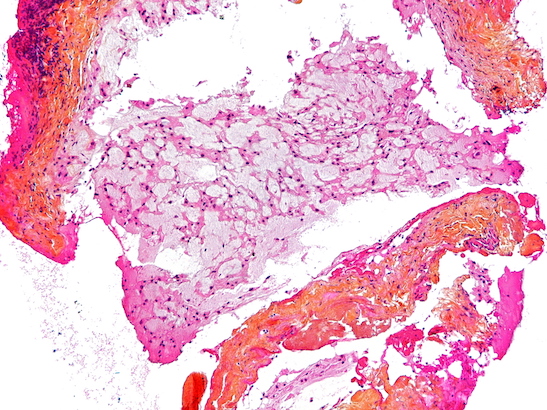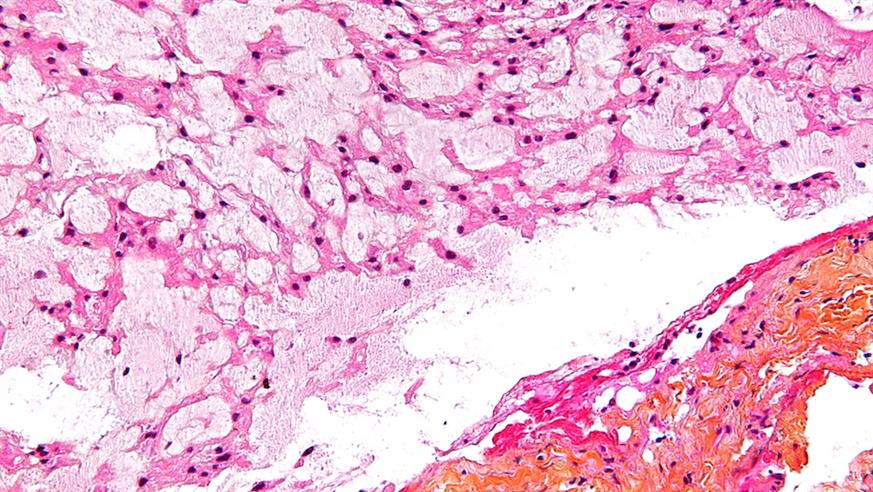
High magnification micrograph of a chordoma. Credit: Copyright © 2010 Michael Bonert. Licence CC BY-SA 3.0.
A study published today in the prestigious journal Nature Medicine identifies a new targeted drug treatment for a rare and difficult-to-treat type of cancer called chordoma which happens to matter a lot to me personally.
I and two of my colleagues here at The Institute of Cancer Research, London, were involved with the international collaborative study, which was led by Dr Tanaz Sharifnia and Professor Stuart Schreiber at the Broad Institute in the US.
The research, which also involved the Chordoma Foundation and other collaborating institutions, was designed with the aim of identifying new therapeutic targets for the treatment of chordoma – a rare primary bone cancer with no approved drug treatment available.
For myself, participation in the study was particularly poignant since my own mother died many years ago as a result of a chordoma tumour.
After having surgery and radiotherapy, there were no drugs available for her and this is still the case for people with the disease today. We hope that this new research will now provide a much-needed treatment option for patients with chordoma.
Urgent need to identify new targets
Chordomas are rare cancers that are thought to arise from the remnants of the notochord – a flexible structure, made out of a material similar to cartilage that disappears in humans during early development of the embryo. Chordomas occur in the base of the skull, the spine and also the sacrum at the base of the spine.
Treatment of chordomas involves surgery and radiotherapy and there are no approved drug treatments – hence the urgent need to identify new therapeutic targets. Unfortunately, this is very challenging because DNA sequencing of chordomas has revealed only very infrequent genetic changes that can be exploited by targeted drugs.
The study team set out to identify potential therapeutic targets by taking two complementary, large-scale screening approaches. The first was to use CRISPR-Cas9 technology to genetically knock out individual genes across the chordoma genome, and the second was to test a library of small-molecule chemicals for activity against chordoma cell lines.
The genetic knockout approach identified a gene (known as T as or TBXT) that encodes a protein called brachyury as being essential for the viability chordoma cell lines, but not for other cancer types. This was interesting because brachyury is a transcription factor – a type of protein that controls the activation of other genes – that has a specific role in the development of the notochord.
Brachyury is not seen in other normal tissues but is abundant in chordoma cells and acts as a ‘biomarker’ for this cancer – helping us to recognise when a tumour is a chordoma.
The brachyury gene is also duplicated in families with an inherited form of chordoma and some sporadic chordomas also have copy number gains for this gene.
Parallel small-molecule screening
All the evidence therefore pointed to brachyury as a possible therapeutic target in chordoma. However, we also knew that, like most transcription factors, brachyury would be extremely difficult to inhibit directly with a drug. It is at this point in the story where the parallel small-molecule screening comes in.
This systematic screen of several hundred compounds identified small-molecules that blocked the division and reduced survival of chordoma cell lines. The library of molecules included those that acted selectively on key nodes in the circuitry of cells and included approved drugs, agents in preclinical development and chemical probes.
Particularly active were inhibitors of enzymes called cyclin-dependent kinase (CDKs) and in fact a subtype of these known as transcriptional CDKs – those that regulate the readout of the genetic code. Further analysis indicated that molecules that inhibited CDKs 7, 12 and 13 or those that blocked CDK9 were most effective against chordoma cells lines.
Why would this be? And what is the connection between the dependence of chordoma cells on CDKs 7/12/13 and 9 and on brachyury?
Inhibiting super-enhancers
Follow-up studies showed that treatment with inhibitors of CDK7/12/13 or of CDK9 reduced the levels of brachyury in chordoma cells – in line with their effects on cell proliferation and survival.
Trancriptional CDKs such as CDK7 are often located in regions of the genome called super-enhancers and inhibitors of these are under clinical investigation because of their ability to reduce the levels of cancer-causing transcription factors.
The study team therefore looked for active enhancers and identified ones associated with the brachyury gene – explaining how the transcriptional CDK inhibitors were reducing brachyury levels and also in fact decreasing the levels of other important gene products regulated in turn by brachyury.
The team also went on to test the effects of other CDK inhibitors. Included in these was a chemical probe inhibitor of CDK8/19 which we provided to the study after identifying it in a previous project with colleagues at Merck KGaA and Cardiff.
This inhibitor was of interest because our previous collaborative work had shown that it too could act on super-enhancers and block the expression of other genes including transcription factors.
However, the results indicated that, in contrast to inhibitors of CDKs 7/12/13 and CDK9, chordoma cells were not sensitive to our CDK8/19 inhibitor, nor were they sensitive to inhibitors of the CDKs that are involved in cell cycle control, such as CDK4/6 inhibitors which have recently shown promise in breast cancer.
These findings helped to demonstrate that only a specific group of transcriptional CDKs, and not others, should be targeted for chordoma treatment.
Potential clinical value of inhibitors
Taken together, the results of the new study reveal a new approach to the management of chordoma involving treatment with small-molecule drugs acting on CDKs 7/12/13 or CDK9 – which work by reducing the levels of brachyury. In support of this, the study showed that an inhibitor of CDKs 7/12/13 was able to block the growth of human chordoma cells growing as a solid tumour in immunosuppressed mice – providing proof of concept for the new approach in an animal model.
Inhibitors of CDK7 and 9 are now undergoing clinical trials and should be evaluated in chordoma patients. In fact, a drug discovered previously by the ICR in collaboration with Cyclacel Pharmaceuticals, CYC065, is one of these.
It was terrific to have the opportunity to contribute to this study with our colleagues at the Broad Institute and elsewhere – showing the value of such collaborations. It wouldn’t have happened if it wasn’t for the great work of the Chordoma Foundation in building a highly collaborative research community around this cancer.
The work not only showed the potential clinical value of inhibitors of the transcriptional CDKs 7/12/13 and CDK9 in chordoma, but also provided a blueprint – involving complementary systematic screening by genetic knockout and small-molecule inhibitors – that can be applied to other cancers where genome sequencing is not able to identify exploitable targets, including rare ones like chordoma.