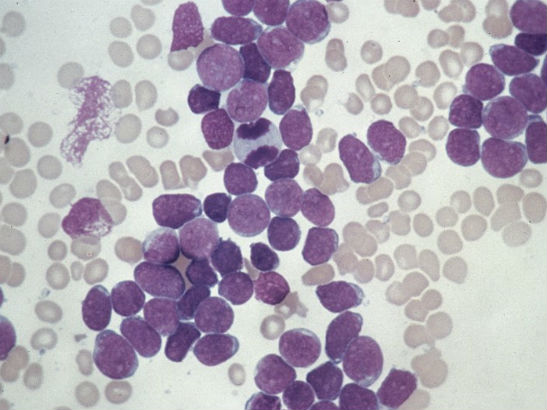
A new study, published in the journal Leukemia, of identical twins with leukaemia has traced its earliest genetic changes all the way back to immature cells from the immune system, which develop before children are even born.
Scientists at The Institute of Cancer Research, London, looked at five pairs of identical twins with acute lymphoblastic leukaemia (ALL), and found that each pair shared an identical, but non-inherited, chimaeric gene made from the fusion of two separate genes called ETV6 and RUNX1.
Previous work by the team at the ICR had shown that the fusion originates in one twin during pregnancy, before spreading to the cells of the other twin through the blood supply of their shared placenta. In this latest study the team used antibody genes to identify the cell type in which the gene fusion arose.
Researchers hope that the new data could start them on the road to understanding how the cells that are affected by the gene fusion develop after birth into fully fledged leukemic cells.
The study, led by the ICR's Professor Mel Greaves, was funded by Leukaemia and Lymphoma Research, with additional support from the Kay Kendall Leukaemia Fund and the Gabrielle’s Angel Foundation for Cancer Research.
Leukaemia is the most common type of cancer in children, and identical twins will often develop leukaemia at the same time, suggesting that there are shared genetic and environmental risks.
Often, the most common genetic mistake seen in twins with ALL is the ETV6-RUNX1 gene fusion, but it has been unclear what cells this fusion gene is acting on.
Genes in our immune system undergo a rearrangement in an early, immature stage, before birth, called the pre-B stage. If identical twins shared the same rearrangements it could suggest that the cells they shared in the womb, with the damagingETV6-RUNX1 gene fusion, might have been pre-B cells.
ICR researchers performed a comprehensive, targeted screen of the bone marrow of five pairs of identical twins with ALL for common rearrangements in their immune system DNA. In every patient, at least two identical genes were found.
In every case, the twins shared both the founder fusion gene, and identical immune cell rearrangements, showing that these mutations did happen early on in the womb, possibly while the pre-B cells were developing in the foetal liver, and were shared between the twins via the placenta.
Study leader Professor Greaves, Professor of Cell Biology at the ICR, said: “It is unusual, and perhaps unique, to be able to identify the likely initiating cell for a cancer in humans, as we have here. By the time someone is diagnosed with cancer, it is usually too late to find out in which cell the cancer developed. Identical twins who suffer from leukaemia can offer us an insight into the root causes of cancer, and an explanation for why some cancers are more difficult to treat than others.”
The team also looked in more detail at one set of twin’s DNA, using a process called single-cell genotyping. They found that, in addition to sharing the fused gene, the twins also shared three single nucleotide variants, and one rearrangement, in every leukemic cell. But their cancers had many distinctive additional mutations, which exist in unique patterns within the cells of their tumours.
This shows that even when two cancers begin with the same trigger and in an identical genetic background they evolve or develop in a distinctive fashion that is specific to each patient.
In the future, the researchers hope to use their insights into leukaemia development to discover the triggers that cause the disease to develop into a clinical condition.