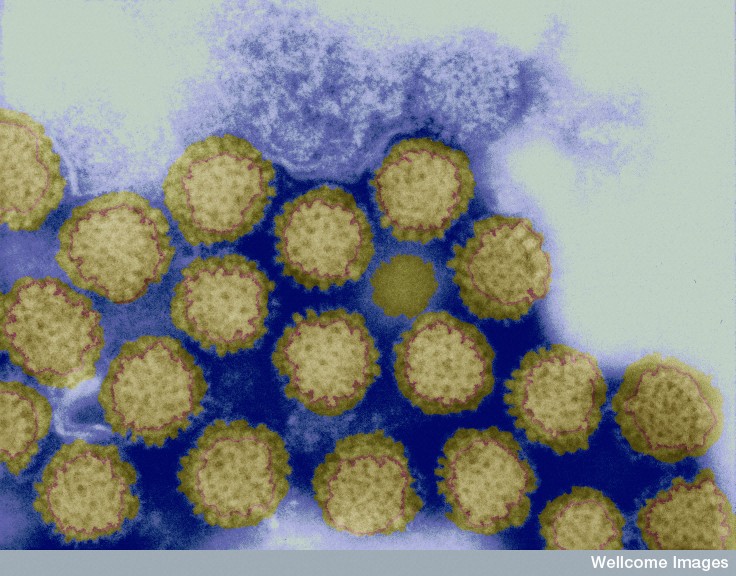
A virus specially designed to target skin cancer boosts the effectiveness of other cancer treatments in an unexpected way, a new study has found
Scientists from The Institute of Cancer Research, London, thought combining the virus with drugs called BRAF inhibitors would boost the virus’s ability to grow in and kill skin cancer cells carrying mutations to the RAS gene.
But they found that the combined treatment had surprisingly little effect in RAS-mutated cancer, and instead worked best in cells with BRAF mutations, a completely unexpected discovery.
In mice with skin cancer, the dual treatment of virus and BRAF inhibitor effectively cured them, with every mouse they studied surviving for more than 60 days.
They were also able to show that RAS-mutated cancers became very susceptible to the virus when it was combined with a different type of drug, called a MEK inhibitor. Both BRAF and MEK inhibitors are now routinely in use in the clinic in patients with skin tumours.
The findings indicate this cancer-targeting virus could be operating in a way not seen before, and using it with other targeted treatments could be even more effective in skin cancer.
The study was published in the journal Molecular Therapy and was funded by Oncolytics Biotech and The Rosetrees Trust, with additional support for some of the laboratory studies from the NIHR Biomedical Research Centre at The Royal Marsden Hospital NHS Foundation Trust and the ICR.
Malignant melanoma is the most aggressive form of skin cancer and is very difficult to treat once it has spread – with chemotherapy having only a 10-20% chance of success. Even with modern drugs that target mutations found in some melanomas resistance is likely to develop, so new approaches are needed.
Cancer-targeting viruses could be an exciting new way to treat melanoma and one such treatment which the ICR has helped to develop is a reovirus These viruses are very common and our cells have developed efficient ways to kill them, but in some types of skin cancer this mechanism is broken.
In cancer with RAS mutations, signals that would destroy the reovirus in healthy cells are blocked, leading to the virus being able to grow and destroy the tumour cells.
Scientists hoped combining reovirus with drugs called BRAF inhibitors might kill more cancer cells by ramping up RAS activity, but in fact the combination treatment did not boost viral replication as expected.
However, when they used the combination in cells with BRAF mutations, they found it was highly effective.
Every mouse with BRAF-mutated skin cancer treated with the combination survived 60 days, compared with 40% of mice that received just the viral treatment.
They found that BRAF inhibitors were causing proteins in a region of the cells to become misfolded, and that this stress led to signals that killed the cancer cells.
The results suggest that combining viral and drug treatment could be an exciting new way to treat malignant melanoma, and one that should be tested out in clinical trials.
Professor Kevin Harrington, Professor of Biological Cancer Therapies at the ICR, said: “Cancer-selective viruses like reovirus, which was developed here at the ICR and The Royal Marsden, could be a powerful new tool to fight malignant skin cancer, but we need ways to increase their potency if we are to truly offer hope to skin cancer patients. By combining the reovirus with a targeted drug called a BRAF inhibitor, we hoped it would boost levels of viral replication in skin cancer cells with RAS gene mutations, but surprisingly we didn’t see this effect.
“Instead what we saw was that BRAF inhibitors and reovirus produced a synergistic effect in skin cancer with BRAF mutations, which was not at all what we were expecting. We were able to work out the mechanism behind this unexpected effect and believe we can use it to our advantage to refine this approach even further. This study is proof of principle that combined treatment could be an effective new therapy for advanced skin cancer and should be studied further in patient trials.”