It’s 15 weeks since the UK entered lockdown to try to control the spread of COVID-19. And although for some, things have started to return to something like normal, it’s becoming increasingly clear that the past 15 weeks have had a lasting impact on many people’s lives.
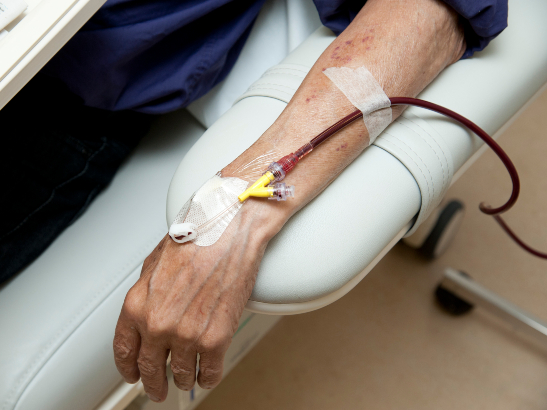
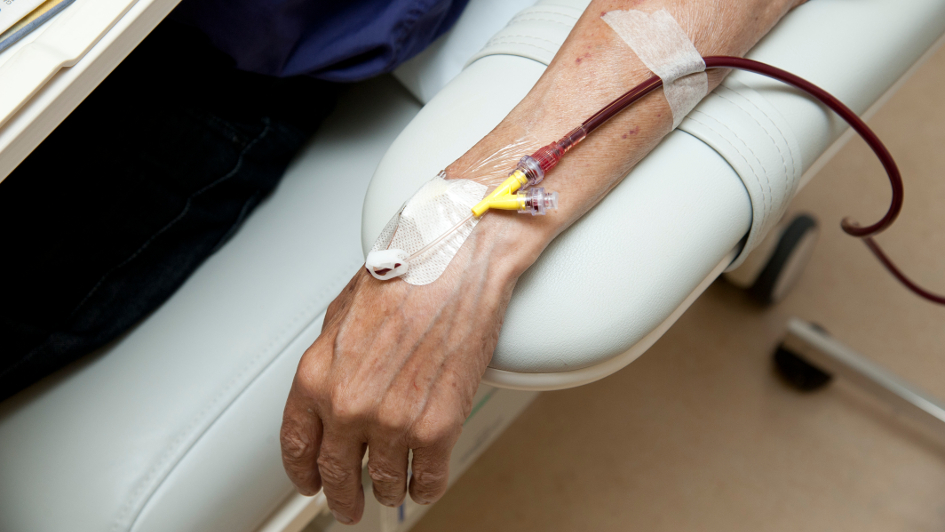
The new coronavirus has had a particularly devastating impact on the delivery of cancer services – as recent ICR-led research has shown. A sobering study, led by Professor Clare Turnbull, helped to kick-start a national conversation after modelling the likely effect of pausing or cancelling cancer treatments because of COVID-19.
It’s a national conversation that is gaining even greater urgency and the subject of Britain’s Cancer Crisis, tonight’s episode of BBC Panorama.
Cancer surgery
For her recent study, alongside working at our partner hospital The Royal Marsden, Professor Turnbull led a team of colleagues at the ICR and other UK universities to assess data on how delays to cancer treatment, particularly to surgery, might affect patients’ survival.
About 95,000 people have a major operation to remove their cancer each year. Surgery in Stage 1-3 cancers is undertaken with the intention of delivering long term cure to the patient. That is, performing the surgery in a 45 year old with the cancer will enable them to live to their normal life expectancy of over 80.
For each month definitive surgical treatment is delayed, the likelihood that the patient will attain long term cure drops. A few months’ delay may be the difference between a life expectancy of 40 years and of two years. The impact of delay varies by tumour type, age of patient and stage of cancer.
About 80,000 of the 95,000 people having a major cancer operation each year are alive at five years post-surgery. Professor Turnbull’s modelling study estimated that if all 95,000 patients experienced three months delay, there would be 4,700 extra deaths within five years of diagnosis. For a universal six months delay, there would be 10,700 extra deaths.
Our research has temporarily been on hold during the Covid-19 crisis, but cancer has not. We need your support to help us make up for time lost in defeating cancer.
Delays
The delay experienced by the patient is the sum of multiple potential delays along the cancer care pathway: delay in presenting to their GP with their symptoms, delay in accessing diagnostic tests such as endoscopy, delay in having cancer surgery and delay in having the chemo- and radiotherapy that may also be required following surgery.
According to the charity Macmillan, urgent GP referrals for suspected cancer in April alone were down 60 per cent, to around 80,000. That equates to around 9,000 missed or delayed cancer diagnoses. Cancer Research UK has said around 2.5 million tests or treatments have been missed because of COVID-19.
Routine cancer diagnostics and surgery have been significantly disrupted on account of concern about infection and diversion of capacity and staff towards acute COVID-19 care.
In parallel to this, normal delivery of cancer care services in the NHS may now be slower on account of new requirements for personal protective equipment (PPE), social distancing and infection control.
The importance of experts
It’s an undeniably grim picture, and underlines the importance of the experts who are quantifying the problem.
That includes academic researchers – like Professor Turnbull and others here at the ICR – whose expertise will help guide our leaders on their strategy as the NHS adapts to a new phase: with restrictions in place to reduce the risk of further peaks in COVID-19, but with greater access to urgent procedures for patients with cancer and other diseases.
It will be an enormous challenge to find the right balance between controlling COVID-19 and ensuring that a stretched NHS can still adequately treat other diseases, for the greatest overall benefit to the greatest number of people. And it’s down to organisations like the ICR to help show the way.
As Professor Turnbull said, announcing the results of the study on delays to cancer surgery, “our findings should help policymakers and clinicians make evidence-based decisions as we continue to deal with the effects of the pandemic on other areas of medicine.
“We have to ensure that both patients with COVID-19 and also those with cancer get the best possible care. That means finding ways for the NHS to get back to normal service on cancer diagnostics and surgery as soon as possible, prioritising certain cancer types in particular.”
BBC Panorama’s Britain’s Cancer Crisis will play an important part in an ongoing national debate about how best to respond to the terrible effect that the COVID-19 pandemic is having on people with cancer.
It’s also set to highlight the determination of the clinicians and researchers whose work will, in spite of the challenging times ahead, help to save countless lives.
Help us kick-start our research
Today, we launched a major fundraising appeal to kick-start our work and make up for the many vital research hours lost to the coronavirus crisis.
In addition to disruption in diagnosing and treating cancer, our research to develop new treatments for cancer patients was put on hold at the start of lockdown, with the majority of our laboratories having to close temporarily to ensure the safety of staff.
While our scientists are now returning to the lab bench, they need urgent support to restart our life-saving research and ensure cancer patients are not left behind.
As funding for research has declined due to cuts in grants and the cancellation of major fundraising events, help to ensure our progress isn’t damaged in the long-term is more important now than ever.
To find out more about the appeal and donate to support our vital research, visit our Kick-start appeal page.